Two separate studies observed the effect that low vitamin D levels had on Teeth, Gums & Heart.
The Journal of Clinical Dentistry (2020) found people with chronic inflammation of the gums (periodontitis), & people who had both periodontitis AND Coronary Heart Disease (CHD) had significantly lower levels of Vitamin D when compared to those with just CHD or healthy people.
In a separate study that observed over 4200 people aged 20 – 80 years, from 2007 – 2008, it was found that Vitamin D levels were significantly associated with the occurrence of tooth decay. The lower the levels, the more tooth decay.
Two Important Concepts Here:
Inflammation in your gums and teeth paired with low vitamin D affects the heart. And low vitamin D is significantly associated with tooth decay and gum inflammation.
Decaying gums and teeth = more bacteria and inflammatory chemicals = affects the immune system = affects the heart. It appears things are seldom separate in the body!
The microbiome starts in the mouth – then goes to the gut – then the intestines – then the colon.
Dr. Stanley Hazen is a brilliant doctor who first mentioned there was a link between gut microbes and heart disease.
While I was scouring through the medical literature to find studies about the Gut-Heart Axis, I found this quote.
In 2014 Dr. Hazen stated, “In the future, we may consider the gut flora to be the largest endocrine organ in the body. Gut flora, depending on the nutrients we consume, makes distinct biologically active substances that act somewhere in the body.”
According to periodontist Dr. Hatice Hasturk of Harvard, “Periodontal disease increases the body’s burden of inflammation, which involves an outpouring of immune cells that attack irritants and microbial invaders — fosters healing over the short term. But chronic inflammation is a key contributor to many health problems, especially atherosclerosis.”
“Daily tooth brushing and flossing can prevent and even reverse an early stage of gum disease, known as gingivitis. If your dentist says you have gingivitis, ask for a brushing and flossing demonstration to make sure you’re doing both correctly.
Many people don’t spend enough time or care when brushing (the recommended duration is two minutes). Flossing sweeps away the sticky film between teeth which leads to plaque buildup. Twice-yearly cleanings by a dentist or hygienist are also advisable.”
“Left untreated, gingivitis can turn into periodontal disease. The gums become loose around the root of the tooth, creating a gum pocket that gradually deepens. Eventually, the infection and inflammation can cause the tooth to loosen and possibly fall out.”
And now, you can add taking Vitamin D to that list!
The Gut-Heart Axis:
In March 2020 I completed my master’s bachelor’s degree in Functional Medicine (woohoo!). I chose to do my thesis paper on the available research on the Gut Heart Axis.
What is the Gut-Heart Axis?
This is the way the microbes in our gut influence the health or disease of the heart.
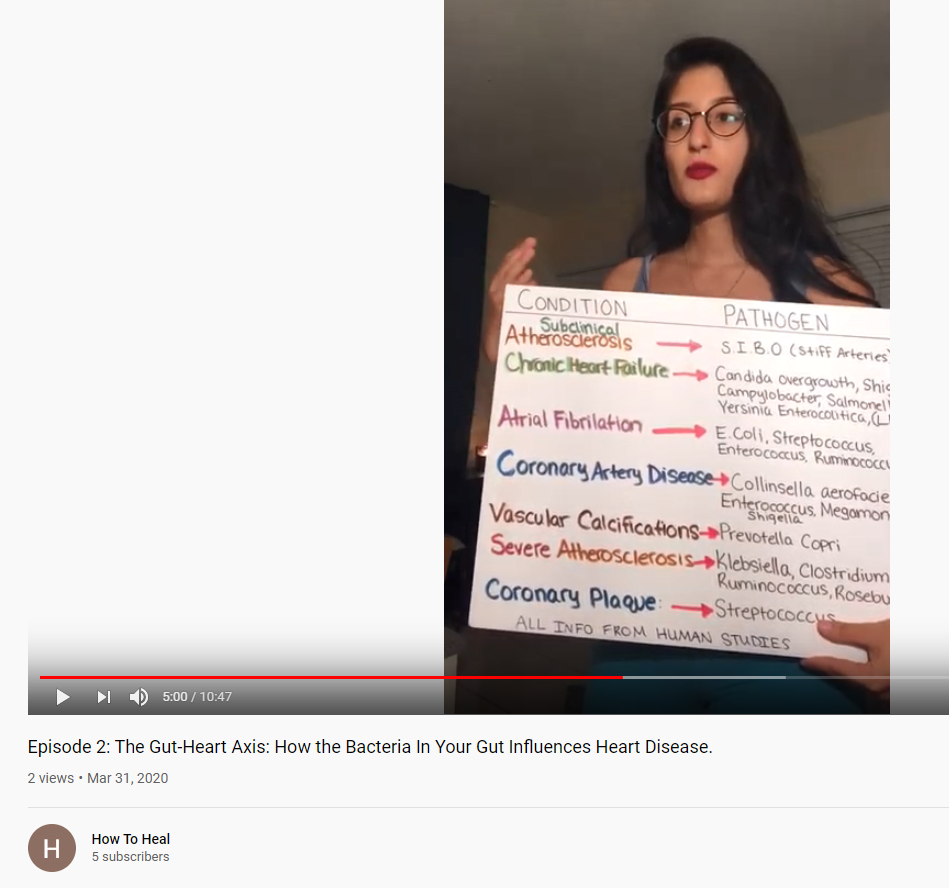
And if probiotics could be used as therapy for the treatment of various heart diseases (including the ones listed to the left in this still shot) and cardiovascular risk factors (high blood pressure, high cholesterol, etc)
I painstakingly (ok, I enjoyed it lol) combed through every bit of literature and human study I could find, and there was NOT a large number of studies.
In fact the majority of the literature I could find dated back to 2017!
I had stumbled upon a novel concept that was probably not being considered by Cardiologists or Gastroenterologists.
Granted, if you go to Cleveland Clinic for major heart surgery, they’re dealing with an emergency situation and wouldn’t say “Okay, take a probiotic and leave.”
But in outpatient facilities, where you are seeing a cardiologist for AFib, Congestive Heart Failure, or you’ve been told that you have a high calcium score, or your carotid arteries are occluded.
What are the chances the doctor would say, You have this heart condition?
I recommend you do a stool test to see if you have an overgrowth of pathogenic bacteria, and this will help us to see how much good probiotic bacteria you have in there as well.”
But, research has shown people with these heart diseases have massive quantities of pathogenic gut bacteria.
One study found people with Small Intestinal Bacterial Overgrowth (SIBO) have a ‘sub-clinical’ atherosclerosis.
Meaning, their arteries weren’t calcified enough to have a high calcium score.
But, they were stiffer and had less pulse wave velocity (the velocity at which the blood pressure pulse propagates through the circulatory system, usually an artery).
Studies Showing Relationship Between Pathogenic Gut Flora and the severity of heart disease.
Below are more fascinating studies finding relationships between pathogenic gut flora and the severity of heart disease.
- A twofold increase in Atrial Fibrillation (AFib) during Irritable Bowel Disease flare-ups. Stroke risk was exclusive to the active IBD flare-ups (Kristensen et al., 2014).
- Chronic Heart Failure (CHF) patients had massive quantities of candida, campylobacter, salmonella, yersinia bacteria, and a 10x increase markers of leaky gut vs. control group. Overgrowth severity was interrelated with increased atrial pressure, inflammation, and venous blood congestion (Pasini et al., 2016).
- SIBO may be a very early indicator of Atherosclerosis and people with SIBO may be at an increased risk for atherosclerosis (Ponziani et al., 2017).
- Vascular calcifications/High Calcium Score: the gut bacteria make vitamin K2/menaquinone-7 (vitamin K2/MK-7), which prevents calcium from depositing on the blood vessel walls. A subclinical Vitamin K2 deficiency can be determined by elevated undercarboxylated MGP (uc-MGP). Elevated uc-MGP is associated with an increased incidence of arterial calcification for which vitamin K2, not K1 supplementation, can improve (Brandenburg et al., 2015)(Gast et al., 2009). MK-7 supplementation significantly decreases calcium from displacing into the arteries.
Probiotics as Therapy for CVD:
I was so impressed with my research and this concept that I’m actually trying to get my paper published in a medical journal.
This research highlights the importance of fusing the fields of Cardiology and Gastroenterology together because they are both interrelated.
Arterial Stiffness:
Multispecies probiotic supplementation can favorably modify vascular dysfunction and reduce arterial stiffness (Szulinksa et al., 2018).
Heart Failure:
Saccharomyces boulardii administered for 3 months significantly reduced cholesterol, improved left ventricle ejection fraction, reduced left atrial diameter, reduced uric acid, reduced inflammatory markers (Costanza et al., 2015).
Hypertension:
Those with hypertension have high amounts of klebsiella, clostridium, and strep bacteria. Those with hypertension also have low amounts of protective short-chain fatty acids.
The more hypertensive the subject is, the more potentially pathogenic bacteria there are (Yan et al., 2017).
Lactobacillus casei supplementation for 2 months showed significant improvements in hypertension and fasting blood glucose (Nakajim et al., 1995).
Probiotics can modulate Angiotensin-Converting Enzyme (ACE), this is a common drug that is given for hypertension, an ACE Inhibitor medication.
Watch a 10 minute summary of my findings on the Gut-Heart Axis click here
Read More Helpful Articles About The Gut
- PROVEN Alternative Ways To Eradicate H. Pylori
- Travel Insurance I & II 60c: Travel without the threat of mosquito, parasite, and bacterial infections
- The Effect of Having Your Gallbladder Removed
- A Deficiency In This Fatty Acid Can Be Causing Your Diabetes, Depression, Weight Gain, & Neurodegen. Diseases.
- Probiotics Improve Major Depressive Disorder